 Fluoride is a mineral that plays an essential role in oral health. In fact, the significant reduction in American tooth decay in recent decades can be attributed to a greater
Read more
Fluoride is a mineral that plays an essential role in oral health. In fact, the significant reduction in American tooth decay in recent decades can be attributed to a greater
Read more
-
Fluoride Use in Adolescents
posted: Apr. 30, 2024.
 Fluoride is a mineral that plays an essential role in oral health. In fact, the significant reduction in American tooth decay in recent decades can be attributed to a greater
Read more
Fluoride is a mineral that plays an essential role in oral health. In fact, the significant reduction in American tooth decay in recent decades can be attributed to a greater
Read more
-
Can You Repair Your Tooth Enamel?
posted: Apr. 23, 2024.
 There are lots of ads out there for toothpastes that claim to repair damaged tooth enamel.
Can you treat cavities and tooth decay at home? Well, mostly, no, you can’t.
Can you
Read more
There are lots of ads out there for toothpastes that claim to repair damaged tooth enamel.
Can you treat cavities and tooth decay at home? Well, mostly, no, you can’t.
Can you
Read more
-
Every Day is Earth Day
posted: Apr. 16, 2024.
 During the early days of the environmental awareness movement, those who demonstrated against pollution, toxic chemicals, and the general public health were known as hippies. The early 1970s were a
Read more
During the early days of the environmental awareness movement, those who demonstrated against pollution, toxic chemicals, and the general public health were known as hippies. The early 1970s were a
Read more
-
Electric or Manual Toothbrush: Why It Does (and Doesn't) Matter
posted: Apr. 09, 2024.
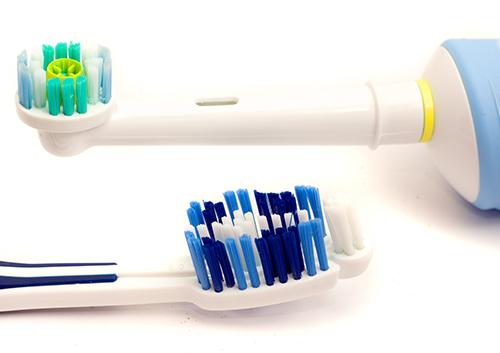 You live in the golden age of toothbrushes. Until a few decades people used twigs or brushes made from animal hair to clean their teeth: not very soft and none
Read more
You live in the golden age of toothbrushes. Until a few decades people used twigs or brushes made from animal hair to clean their teeth: not very soft and none
Read more
-
April is Oral Cancer Awareness Month
posted: Apr. 02, 2024.
 What is oral cancer?
April is Oral Cancer Awareness Month. If you have been putting off a visit to our Batavia, Illinois office, now is an excellent time to schedule
Read more
What is oral cancer?
April is Oral Cancer Awareness Month. If you have been putting off a visit to our Batavia, Illinois office, now is an excellent time to schedule
Read more
-
Alleviate Tooth Sensitivity
posted: Mar. 26, 2024.
 If a sip of ice water, spoonful of ice cream, or piping hot latte is enough to send shivers up your spine from tooth sensitivity, be assured you are not
Read more
If a sip of ice water, spoonful of ice cream, or piping hot latte is enough to send shivers up your spine from tooth sensitivity, be assured you are not
Read more
-
Weighing the Facts about DIY Scaling
posted: Mar. 19, 2024.
 The dental section of your local drugstore or favorite online site offers more dental tools for home care than ever before. Little angled mirrors. Tongue scrapers. Gum stimulators. Interproximal brushes.
Read more
The dental section of your local drugstore or favorite online site offers more dental tools for home care than ever before. Little angled mirrors. Tongue scrapers. Gum stimulators. Interproximal brushes.
Read more
-
Going Green for St. Patrick’s Day?
posted: Mar. 12, 2024.
 Happily for all of us who like to celebrate with friends and family, there’s no need to be Irish to enjoy St. Patrick’s Day. Every March 17th, many of us
Read more
Happily for all of us who like to celebrate with friends and family, there’s no need to be Irish to enjoy St. Patrick’s Day. Every March 17th, many of us
Read more
-
Are your teeth ready for the big day?
posted: Mar. 05, 2024.
 Capturing the Moment
At Fox River Dental Batavia we know that just about anyone who has taken on the challenge of planning her own wedding could tell you how important the
Read more
Capturing the Moment
At Fox River Dental Batavia we know that just about anyone who has taken on the challenge of planning her own wedding could tell you how important the
Read more
-
Dental Insurance Benefits
posted: Feb. 27, 2024.
 Dental insurance can be a great addition to your health care plan, but the way benefits are calculated can also make it a confusing one. If you have dental insurance,
Read more
Dental insurance can be a great addition to your health care plan, but the way benefits are calculated can also make it a confusing one. If you have dental insurance,
Read more
-
Anatomy of a Smile Makeover
posted: Feb. 20, 2024.
 A smile makeover is usually a combination of one or more cosmetic dental procedures. To achieve your desired result, the doctor may perform or suggest a variety of options. The
Read more
A smile makeover is usually a combination of one or more cosmetic dental procedures. To achieve your desired result, the doctor may perform or suggest a variety of options. The
Read more
-
Valentine's Day History
posted: Feb. 13, 2024.
 Valentine’s Day is best known as a celebration of love in all its forms. Pink hearts, red roses, and cute greeting cards adorn every surface you see. What many people
Read more
Valentine’s Day is best known as a celebration of love in all its forms. Pink hearts, red roses, and cute greeting cards adorn every surface you see. What many people
Read more
-
Courting Disaster
posted: Feb. 06, 2024.
 When we think of sports and dental damage, we naturally think of hockey and football. But when it comes to the actual number of dental injuries suffered each year, vying
Read more
When we think of sports and dental damage, we naturally think of hockey and football. But when it comes to the actual number of dental injuries suffered each year, vying
Read more
-
It's been years since my last appointment; what should I expect?
posted: Jan. 30, 2024.
 Feeling apprehensive or guilty for not visiting a dentist in over a year is common, but coming back to receive dental care is easier than you may think. Our dental
Read more
Feeling apprehensive or guilty for not visiting a dentist in over a year is common, but coming back to receive dental care is easier than you may think. Our dental
Read more
-
Protect Your Baby from Early Childhood Caries
posted: Jan. 23, 2024.
 Your baby’s first smiles are precious—and you want to make sure those precious smiles are as healthy as they are beautiful. One of the most important ways to protect your
Read more
Your baby’s first smiles are precious—and you want to make sure those precious smiles are as healthy as they are beautiful. One of the most important ways to protect your
Read more
-
My gums are inflamed. What can I do?
posted: Jan. 16, 2024.
 Inflamed gums are a fairly common dental issue, but unfortunately, many people don't take the problem seriously enough. If you ignore inflamed gums and continue your usual routine, you could
Read more
Inflamed gums are a fairly common dental issue, but unfortunately, many people don't take the problem seriously enough. If you ignore inflamed gums and continue your usual routine, you could
Read more
